SCOLIOSIS:
TO EXERCISE OR NOT
by: Andrea
S. Ruark
Will exercise or spinal manipulations
prevent scoliosis from progressing?
Will these things correct already diagnosed
scoliosis? Are there any activities
a child or adolescent with scoliosis
cannot do? Defining scoliosis, classifying
scoliosis, and learning about different
methods of treatment can help answer
these questions.
 According
to Stopka & Todorovich (2005), “Scoliosis
is a lateral curvature, accompanied
by vertebral rotation of the spinal
column (p57).” Many schools perform
routine scoliosis screenings in middle
and high school. A forward bending test
is used to look for symmetry between
the left and right side of the spine.
An observer stands behind or in front
of the student while the child bends
forward toward their knees and toes. According
to Stopka & Todorovich (2005), “Scoliosis
is a lateral curvature, accompanied
by vertebral rotation of the spinal
column (p57).” Many schools perform
routine scoliosis screenings in middle
and high school. A forward bending test
is used to look for symmetry between
the left and right side of the spine.
An observer stands behind or in front
of the student while the child bends
forward toward their knees and toes.
The observer examines the region between
the upper thoracic and lumbar regions
of the spine. If the observer sees anything
that appears asymmetrical, the child
is referred to their primary physician
for further diagnosis. Examples of asymmetrical
findings include one shoulder higher
than the other, a “winged”
scapula,
or a rib hump on one side, uneven waist,
leaning to one side, and one hip higher
than the other (Staff, 2007).
Scoliosis curves can be identified
as functional or structural. Functional
curves resolve when the cause of the
curve is rectified (Lonstein, 1999).
Examples include leg length discrepancies
that are fixed with a heel lift, or
ruptured discs that are repaired through
physical therapy or surgery. Structural
curves have three main causes; congenital
scoliosis, neuromuscular
scoliosis, or idiopathic
scoliosis (Lewis, 2008).
Congenital scoliosis is present
at birth, and means the vertebrae did
not form correctly or the ribs fused
during fetal development. Neuromuscular
scoliosis is caused by muscle weakness
or paralysis due to disease. Possible
disease causes are cerebral palsy, muscular
dystrophy, and polio. Idiopathic
scoliosis is from an unknown cause
and includes the majority of adolescent
scoliosis diagnoses. According to Yochum
& Maola, “Of all causes, an
inherited genetic defect appears to
play a significant role with up to 30
percent of patients having another family
member with significant scoliosis (p14).”
However, this genetic link does not
appear to determine the progression
or severity of the curve (Yochum D.C.
& Maola D.C., 2008).
 A
physician typically uses three diagnostic
steps. These include a physical examination
of the spine, shoulders, hips, and legs,
including the forward bending test,
x-rays, and possibly an MRI.
The doctor uses the x-ray to calculate
the degree of the spinal curvature,
and determines the treatment based on
this, the child’s age, and where
the child is in their growth spurt.
An MRI is only used if the x-ray shows
something abnormal, or the physical
exams shows neurologic changes (Lewis,
2008). A
physician typically uses three diagnostic
steps. These include a physical examination
of the spine, shoulders, hips, and legs,
including the forward bending test,
x-rays, and possibly an MRI.
The doctor uses the x-ray to calculate
the degree of the spinal curvature,
and determines the treatment based on
this, the child’s age, and where
the child is in their growth spurt.
An MRI is only used if the x-ray shows
something abnormal, or the physical
exams shows neurologic changes (Lewis,
2008).
After diagnosing scoliosis, the physician
describes the curve according to its
shape, C-or S-shaped; the location of
the curve, thoracic,
lumbar,
or thoracolumbar;
the direction of the curve, left or
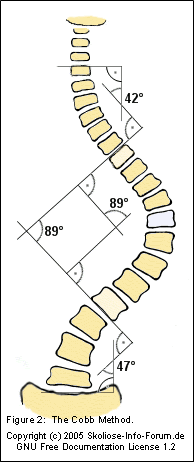
right; and the angle of the curve. The
degree of each curve is measured by
the Cobb
method (see figure 2). The Cobb
method determines the angle of the curve
by measuring the angle between the two
most slanted vertebrae (Lonstein, 1999).
Scoliosis is identified as a curve larger
than 10 degrees, regardless of spinal
level.
According to the Mayo Clinic, when
considering treatment, physicians look
at six different risk factors for progression
(Staff, 2007). The first of these factors
is growth. A growth spurt often worsens
an existing curve. A second factor is
sex; scoliosis in girls is more likely
to worsen than scoliosis in boys. The
age of a child also contributes to the
progression of a curve. If a child is
very young when scoliosis is identified,
chances are the curve will increase.
Size of the curve is a fourth factor:
the larger the angle of the curve, the
more likely that it will worsen.
The location of the curve also determines
the potential for progression. Curves
in the thoracic region are more likely
to worsen than those in the lumbar or
thoracolumbar region. A final determinant
for progression is whether there were
spinal problems at birth. Congenital
scoliosis is more likely to progress
than other types of scoliosis.
Treatment for scoliosis is based mainly
on the degree of the curve, how quickly
the curve is progressing, and where
the child is in their growth spurt.
According to Lonstein (1999), “If
a curve is less than 20 degrees, an
increase in the curve of 10 degrees
or more is required before bracing is
started. A 20 – 29 degree curve
must change by five degrees before treatment
is initiated. A curve between 30 and
40 degrees requires immediate bracing
if the child is still growing. If a
curve is between 40 degrees and 100
degrees, surgery is typically indicated
(p. 599).”
There are three types of braces commonly
used in scoliosis, the Boston
brace, the Milwaukee
brace, and the Charleston
Bending brace. Bracing is only effective
if the skeleton of the child is not
mature. For girls, the skeleton is mature
between the ages of 15 and 16 years,
and for boys the skeleton is mature
between the ages of 17 and 18 years.
The Boston
brace is also called a thoraco-lumbo-sacral-orthosis,
and is often referred to as an “underarm”
brace. This brace works by applying
three points of pressure to the curve
to prevent progression. The most common
application is for curves in the lumbar
or thoraco-lumbar spine. The brace is
made out of hard plastic that has been
molded to the child’s body. It
is worn 23 hours a day, but can be removed
for gym class, swimming and other sports.
The Milwaukee
brace is a cervico-thoracic-lumbo-sacral-orthosis.
This brace looks like the other brace,
but has a neck ring that is attached
to the body of the brace to hold it
in place. Like the Boston brace, this
one is worn 23 hours a day and can be
removed during the day for physical
activity. This brace is suggested for
thoracic spine curvatures. A final brace
is the Charleston Bending brace (figure
4).
The Charleston
brace is molded to the child’s
body when they are bent toward the convexity
of the curve, thus applying more pressure
to the curve (McAffee, 2002). Because
the brace is only worn at night, many
self-esteem issues are avoided. Self-consciousness
due to wearing a brace at school, or
a student’s friends “finding
out” is avoided. This brace is
recommended for curvatures of 25-40
degrees with the apex of the curve below
the height of the shoulder blade (McAffee,
2002).
 Surgical
intervention is required for curvatures
between 40 degrees and 100 degrees.
According to the Mayo Clinic, “Scoliosis
surgery is one of the longest and most
complicated orthopedic surgical procedures
performed on children (Scoliosis: Surgery).”
The operation lasts approximately six
hours and requires a 5-7 day hospitalization.
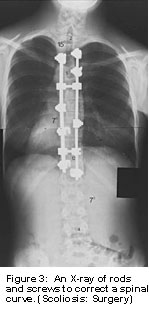
Mayo clinic surgeons perform a posterior
spinal fusion that uses a modified two-rod
system originally invented in 1984 by
two French surgeons. The rods and screws
are attached to the spine in an effort
to correct the curve as much as possible
(figure 5). Part of the spine fuses
to maintain the correction. The hardware
is not removed, even after the fusion
is healed. A person’s movement
may be slightly altered. Surgical
intervention is required for curvatures
between 40 degrees and 100 degrees.
According to the Mayo Clinic, “Scoliosis
surgery is one of the longest and most
complicated orthopedic surgical procedures
performed on children (Scoliosis: Surgery).”
The operation lasts approximately six
hours and requires a 5-7 day hospitalization.
Mayo clinic surgeons perform a posterior
spinal fusion that uses a modified two-rod
system originally invented in 1984 by
two French surgeons. The rods and screws
are attached to the spine in an effort
to correct the curve as much as possible
(figure 5). Part of the spine fuses
to maintain the correction. The hardware
is not removed, even after the fusion
is healed. A person’s movement
may be slightly altered.
A second type of surgery that Mayo
clinic surgeons are investigating is
for early onset scoliosis (Scoliosis:
Surgery). This technique uses “growing
rods.” Two parallel rods are attached
at each end of the curve. As the term
“growing rods” implies,
the center of the rods are adjustable
as a child grows. The lengthening of
the rods is done during outpatient surgery.
This surgery helps prevent heart and
lung difficulties associated with early
onset scoliosis.
Other treatments for scoliosis include
neuromuscular electrical stimulation
of muscles, chiropractic manipulation,
and physical therapy. Limited information
is available on the use of these methods
to treat or prevent scoliosis. Clinical
trials using neuromuscular electrical
stimulation of muscles alone to correct
a scoliosis curvature, or to prevent
the progression of a curve, have not
been published. A type of trial published
in a 2001 issue of the Journal of Manipulative
and Physiological Therapeutics reports
in their study, spinal manipulations
alone, “…were not effective
in the correction of curvature of scoliotic
spines… (Lantz D.C. & Chen
D.C., 2001).”
However, a case study done by Kao-Chang
Chen, M.D. and Elley H.H. Chiu, M.D.
in The Journal of Alternative and Complimentary
Medicine used chiropractic manipulation
to decrease a Cobb angle of 460 to 300
in a 15 year old girl after 18 months
of intervention (p. 749). A literature
review by Martha C. Hawes, published
in Pediatric Rehabilitation “…supports
the hypothesis that exercise-based therapies
can be used to reverse the signs and
symptoms of scoliosis in children and
adults (p. 178).” The review also
points out that, “…there
does not appear to be a single study
supporting the dogma that scoliosis
will not respond to exercise-based therapies
applied early in the disease process
(p. 178).”
Physical activity is not limited for
adolescents with scoliosis that are
receiving brace treatment, physical
therapy, or chiropractic. The brace
can be taken off for physical activities
that require more flexibility, or for
contact sports or swimming. Physical
activity is only contraindicated for
adolescents that have had surgery. Each
doctor will likely have their own protocol,
but the Mayo Clinic’s protocol
for post-surgical fusion follows these
activity guidelines. Post-surgery includes
a restriction of activities for several
days, and a restriction from physical
activities like running and gym class
for three months after surgery.
According to the Mayo clinic’s
protocol, patients can return to normal
activity excluding gym class, diving,
contact sports, horseback riding, amusement
park rides and lifting more than 25
pounds after three months (Scoliosis:
Surgery). After six months, the patient
can rejoin gym class and participate
in all activities except contact sports
with their doctor’s permission.
One year after surgery without complications,
and with their doctor’s permission,
a patient can return to full activity
including contact sports.
Although the literature supports varying
theories on the effectiveness of bracing,
surgery, chiropractic manipulation,
and physical therapy, it seems clear
that most adolescents with idiopathic
scoliosis can lead a full, active life.
Children with scoliosis can participate
in school sports, recreational sports,
and individual activities during treatment
for scoliosis. And students that have
surgery to correct a scoliosis curve
can resume participation in most activities
after six months and full activity after
a year.
Works
Cited
Chen, K.-C., & Chiu, E. H. (2008).
Adolescent Idiopathic Scoliosis Treated
by Spinal Manipulation: A Case Study.
The Journal of Alternative and Complementary
Medicine , 749-751.
Hawes, M. C. (2003). The use of exercises
in the treatment of scoliosis: and evidence-based
critical review of the literature. Pediatric
Rehabilitation , 171-182.
Lantz D.C., C. A., & Chen D.C.,
J. (2001). Effect of Chiropractic Intervention
on Small Scoliotic Curves in Younger
Subjects: A Time-series Cohort Design.
Journal of Manipulative and Physiological
Therapeutics , 385-393.
Lewis, R. A. (2008, February 27). Medical
Encyclopedia: Scoliosis. Retrieved
March 22, 2009, from Medline Plus: http://www.nim.nih.gov/medlineplus/ency/article/001241.htm
Lonstein, J. E. (1999). Scoliosis update:
Managing school screening referrals.
Journal of Musculoskeletal Medicine
, 593.
McAffee, P. C. (2002, March 26). Types
of Scoliosis Braces. Retrieved
March 28, 2009, from Spine Health: http://www.spine-health.com/conditions/scoliosis/types-scoliosis-braces
Scoliosis: Surgery. (n.d.). Retrieved
March 28, 2008, from MayoClinic.com:
http://www.mayoclinic.org/scoliosis/surgery.html
Staff, M. C. (2007, December 14). Scoliosis.
Retrieved March 22, 2009, from MayoClinic.com:
www.mayoclinic.com/health/scoliosis/DS00194
Stopka, C., & Todorovich, J. R.
(2005). Applied Special Physical
Education and Exercise Therapy.
Boston: Pearson Custom Publishing.
Yochum D.C., T. R., & Maola D.C.,
C. J. (2008). Scoliosis. The American
Chiropractor , 14-16.
|



